Introduction: Use of validated risk stratification tools for work up of suspected pulmonary embolism (PE) is an endorsed recommendation of the American Society of Hematology and the American College of Emergency Physicians. Due to variations in clinical practice, electronic health record (EHR) systems, and medical provider trainings, the use, documentation, and implementation of these tools vary widely. Current processes do not allow for electronic capture and quality reporting at most institutions.
Methods: We sought to design and implement clinical pre-test probability (PTP) tools at three large healthcare institutions for use in emergency departments (ED). At each site, a hematologist partnered with ED physician leadership and local information technology experts to design and implement PTP tools in clinical workflows. Overall, 38 EDs (high volume tertiary EDs and smaller regional EDs) located in the United States along the East Coast and Midwest regions were involved. A major goal of implementation was integration into clinical workflow and automatic documentation. After design and implementation, awareness and education of the new EHR tool was distributed electronically to ED providers. After implementation, use of PTP tools was analyzed between September 12, 2022 and January 11, 2023. PTP use was examined as percent of visits for which patients underwent CT pulmonary angiography (CTPA).
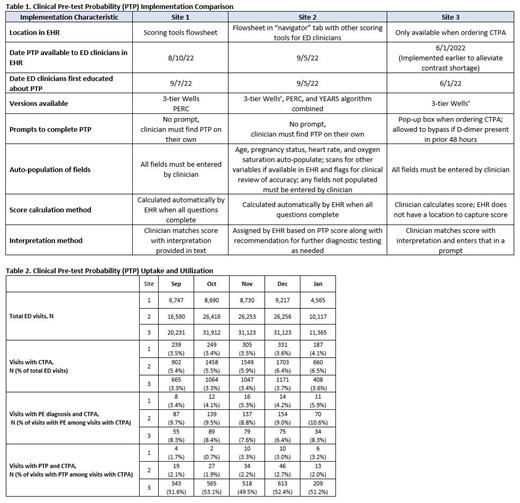
Results: Each institution chose the 3 tier Wells' Score for implementation while one site designed an integrated Wells'/PERC or YEARS score calculator. Two sites implemented the tool as an optional flowsheet and one site implemented the tool as mandatory parameters within the orders for PE imaging studies. The mandatory tool could be bypassed with prespecified selections or if a D-dimer existed within 48 hours . Complete details of the site-specific implementation are shown in Table 1. Over the 4-month evaluation timeframe, there was a total of 270,214 ED encounters. Uptake and utilization of the PTP tools are shown in Table 2. Use of PTP was highest at the site with forced PTP documentation which ranged from 49-53% of ordered CTPAs, compared to Site 2 where use was 2-3%, and Site 1 where use ranged from 1-3%. At Site 1, use of PTP increased slightly over the study period with signs that PE yield on imaging was increasing as well (3.4% to 5.9%). At Site 2, PE yield on imaging was overall high (9-10%), and remained similar with similar use of PTP tools over the study period. Use of PTP and PE yield (6-8%) on imaging also remained similar throughout the study at Site 3.
Conclusion: Forced use of PTP within the orders for CTPA led to the highest use of PTP (Site 3) but this did not result in meaningfully higher PE yield on CTPA compared to the other sites. PE yield at each site was at or above the 5% yield for PE on CTPA which has been previously reported. Given that PTP uptake was relatively stable over the measurement period at Site 2 and 3, this indicates the process had mostly stabilized and that other strategies are needed to improve uptake of PTP, reduce utilization of CTPA, and further increase yield on CTPA. Increasing PTP use and rising PE yield at Site 1 demonstrated ongoing potential for improvements past this study timeframe.
Disclosures
Rosovsky:Inari: Consultancy; Pulmonary Embolism Response Team: Membership on an entity's Board of Directors or advisory committees, Other: President-Elect; BMS: Consultancy; Dova: Consultancy; Janssen: Consultancy, Other: Research funding is to my institution, Research Funding; Abbott: Consultancy; Penumbra: Consultancy, Other: National Lead Investigator for STORM PE.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal